Therapy at a pace your system can stay with
Relational, body-aware psychotherapy for anxiety, overwhelm, stuckness, relationship difficulties, and recurring ways of coping shaped by stress, past experience, or trauma.
Sessions are available in person in Shinfield, Reading, Berkshire, and online.
You may be reaching out because of emotional shutdown, disconnection, painful relationship patterns, or a sense that things are not shifting despite insight, effort, or previous therapy.
Emotional shutdown can sometimes feel like going blank, withdrawing, losing access to words, functioning on the outside while feeling collapsed inside, or entering a protective shutdown mode when stress, closeness, or pressure becomes too much.
When insight has not been enough
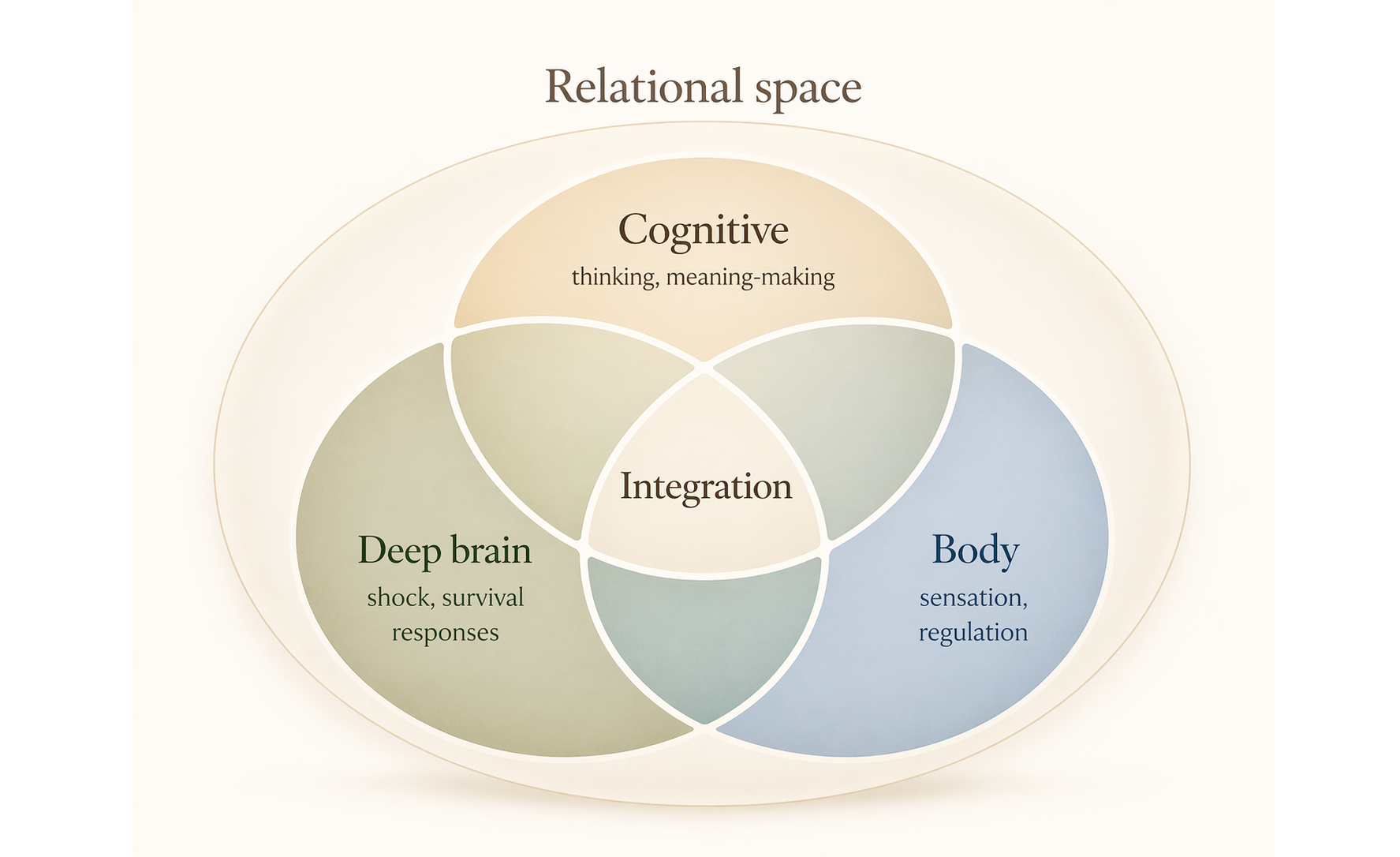
My approach is relational and body-aware, with attention to both the mind and the nervous system.
This may be particularly relevant if you are looking for a psychotherapist in Reading or online for anxiety, trauma, or patterns that have been difficult to shift.
The work may draw on approaches such as Deep Brain Reorienting (DBR), Sensorimotor Psychotherapy, parts-informed work, and EMDR-informed work. These are not applied as a fixed formula, but used where they genuinely fit the person, the work, and the pace your nervous system can stay with.
This can be especially helpful when difficulties show up as chronic stress, hypervigilance, dissociation, sleep disruption, fatigue, brain fog, shame, or people-pleasing.
It may also be a good fit if you have tried to understand or change these patterns, but still find yourself pulled back into old protective responses when stress, closeness, or uncertainty rises.
This may be for you if
You may recognise that:
anxiety, shutdown, shame, or overwhelm keep returning
relationship patterns feel difficult to shift
you understand some of what happens, but still react automatically under stress
your body seems to stay on alert, collapse, or disconnect
you are looking for therapy that is careful, relational, and deeper than symptom management alone
“I’d spent years understanding why I reacted the way I did. Working with Paolo was the first time something began to shift.”
— Former client, anonymised
A first conversation can help you find a starting point
You do not need to know exactly where to begin. A free 20-minute consultation is a chance to talk briefly about what is happening, what you are looking for, and whether this way of working may be a good fit.
How we begin
We begin by building a therapeutic relationship that feels steady enough to work in. That relationship is part of what makes the work possible.
Early on, therapy is usually about understanding what is happening: what brings you here, what helps, what destabilises you, and what may need to change.
We may then agree an initial therapeutic direction, including what to prioritise, how to support regulation where needed, and how we will review progress.
The process stays collaborative, with attention to pacing, consent, and honest feedback.
What to expect in sessions
Early sessions usually focus on helping life feel more manageable. Together, we make sense of what you are experiencing, notice patterns and triggers, and identify what helps between sessions.
Sessions may include talking, reflecting on relationship patterns, noticing bodily responses, working with emotions as they arise, or reviewing what feels different between sessions. The balance depends on what you need and what your system can manage.
Some sessions are more practical. Others move into deeper work when there is enough capacity for that.
We keep paying attention to what helps and what feels too much.
How the process usually unfolds
An initial phase of the work
If appropriate, we begin with a short initial phase, often around 4–6 sessions. During this time, we explore your current difficulties, relevant life history, and what helps you stay within a tolerable range.
By the end of this phase, I aim to offer a clear initial therapeutic plan tailored to you, including priorities and how we will review progress.
Stabilisation first, when needed
When the nervous system is under significant strain, stabilisation often comes first.
This means helping things settle enough for daily life to feel steadier, more manageable, and more workable. Where trauma-driven responses are involved, body-based, bottom-up work often provides the foundation for deeper therapy.
Deeper work and integration
As stability improves, deeper work often becomes more tolerable and effective.
This may include working with unresolved trauma, relational patterns, protective responses, self-criticism, shame, grief, or parts of the self that have had to adapt under pressure.
In my practice, deeper work is not about forcing disclosure or pushing into overwhelming material. It is about working carefully with what is ready to be met, so that change can happen without flooding, collapse, or shutdown.
As this begins to shift, people often find more room for rest, clarity, and connection, and a greater sense of responding from the present rather than from old protective patterns.
Over time, therapy may also support wider growth, including:
more choice and flexibility in daily life
less pull towards old reactions
greater capacity to feel without becoming overwhelmed or shut down
more self-trust and self-compassion
clearer boundaries and more satisfying relationships
If trauma, chronic stress, or nervous-system strain feel central to what you are living with, you may also wish to read more on the Trauma page ›
Approaches I integrate
My primary training is in Relational Transactional Analysis, and I integrate additional approaches where helpful.
These approaches sit within one relational, trauma-informed process and are used where they genuinely fit the person, the work, and the pace your nervous system can stay with.
Depending on your needs, this may include:
Deep Brain Reorienting (DBR)
Sensorimotor Psychotherapy
parts-informed work
EMDR-informed work
DBR is a core component of my trauma work.
If you would like a clearer sense of the approaches I integrate and how they are brought together within one way of working, you can read more here:
Approaches I integrate in therapy ›
Read more:
Neurofeedback alongside psychotherapy
For some people, adding ILF neurofeedback in person can support stabilisation, particularly with sleep, arousal regulation, emotional reactivity, and overall self-regulation.
I usually offer ILF neurofeedback within an ongoing psychotherapeutic process. Where clinically appropriate, this may also be complemented by frequency-based neurofeedback training.
This may be useful when sleep difficulties, overwhelm, high reactivity, or difficulty settling are making daily life — and psychotherapy itself — harder to manage.
At other times, psychotherapy on its own may be the better place to begin. The question is whether neurofeedback is likely to be helpful at this stage.
We review neurofeedback at agreed points, adjusting according to sleep, arousal, and overall stability.
Read more about ILF neurofeedback ›
For common questions about starting therapy, how the process works, and what to expect, the FAQ may be helpful ›
Practicalities
Adults aged 16+
In person in Shinfield, Reading, Berkshire
Online via Zoom
Sessions are typically 50 minutes, usually weekly
Fees: Fees ›
Is this the right fit?
Some people come with a clear sense of what they want to work on. Others arrive unsure, and we begin there.
My way of working is exploratory, relational, and often longer-term. It tends to suit people looking for something more than symptom relief or a purely structured, skills-based approach.
If this way of working feels relevant, you are very welcome to book a free 20-minute consultation.
We can talk about what is happening day to day, what you would like to feel more possible, and whether working together seems likely to help.
If it does not seem like the right fit, I will say so honestly and help you think about alternatives.
There is no pressure to continue beyond the consultation.