When the body still responds as if danger is near
Sessions are available in person in Shinfield, Reading, Berkshire, and online.
If trauma, chronic stress, or nervous-system strain may be part of what you are living with, this may be a helpful place to begin.
When your mind understands but your body still reacts, therapy can help you work with what your system learned to do under pressure — and what may still be carried now.
You may feel anxious, on edge, shut down, disconnected, easily overwhelmed, or unable to fully settle. You may also notice that something in you still responds as though safety cannot quite be felt yet.
Trauma does not always look dramatic from the outside. It may show up through anxiety, shutdown, self-protection, people-pleasing, dissociation, poor sleep, relationship difficulties, or a body that still expects to stay ready.
It can also show up relationally — in finding it hard to trust, losing your words under pressure, withdrawing quickly, trying hard to keep the peace, or finding that closeness and care feel harder to tolerate than you want them to.
Insight matters. And when trauma is carried in the body and nervous system, understanding alone is often not enough.
In therapy, I do not force change. We begin with stabilisation, capacity, and a pace your system can stay with. When you are ready, we may move into trauma processing and longer-term therapeutic work.
This may be for you if
You may recognise that:
your mind understands something, but your body still reacts
anxiety, shutdown, dissociation, or hypervigilance take over under stress
closeness, conflict, or uncertainty can feel unexpectedly threatening
you find yourself people-pleasing, withdrawing, bracing, or trying to stay in control
previous therapy or insight helped, but did not fully change the pattern
If what feels most familiar is the shape of your symptoms and experience, rather than the word trauma itself, you may also find Symptoms & experiences helpful.
“What made the difference was the pace. I did not feel pushed, and that helped me stay with things I would usually have avoided or shut down around.”
— Former client, anonymised
Over time, this can help life feel less organised around survival and more open to rest, steadiness, and connection.
Recognising trauma responses
Trauma often shows up as a nervous system that struggles to settle, soften, or feel safe.
Some people live more in a state of high alert: scanning, bracing, startling easily, or finding it hard to relax. Others are pulled into shutdown: numbness, fog, sleepiness, collapse, or a sense of being unable to mobilise.
Some people experience waves of panic. Others feel unreal, distant, or disconnected from themselves or their body. Sleep, concentration, appetite, energy, and emotional balance may all be affected.
For many people, the impact is relational: people-pleasing, withdrawal, conflict cycles, difficulty trusting, or feeling unsafe with closeness. Trauma can also shape confidence, self-worth, identity, boundaries, and the sense of having a right to take up space.
When threat is experienced, the body often responds before there is time to think. The nervous system may move into fight, flight, freeze, collapse, submit, or appease. These are survival responses, not signs of weakness or failure.
You might recognise patterns such as:
going numb or not feeling much
staying busy to avoid what you feel
perfectionism, self-criticism, or over-responsibility
withdrawing, avoiding, or people-pleasing
pushing through until you crash
needing control in order to feel safer
feeling responsible for other people’s emotional states
finding rest difficult, even when exhausted
None of these is a personal failing. They are adaptations — signs that your system did what it needed to do.
The work is not to criticise these responses, but to understand them, respect their protective function, and help the system gradually find more choice.
Why trauma affects people differently
The impact of trauma is not only about what happened.
It is also shaped by the context around it: how long it went on, whether it happened once or repeatedly, whether it happened in childhood or adulthood, whether it involved people who were meant to provide care, and whether there was enough support afterwards.
Trauma may take different forms. Shock trauma may involve a sudden overwhelming event or short period of acute danger.
Developmental, attachment, or relational trauma may involve earlier experiences that shaped safety, identity, connection, and emotional regulation over time.
Cumulative trauma may involve repeated experiences that gradually organise the nervous system around protection, vigilance, appeasement, or shutdown.
A single overwhelming event can have a lasting impact. Repeated, relational, or developmental trauma can shape the nervous system more gradually, especially when there was little room to protest, escape, be believed, or receive protection.
Some experiences may not look severe from the outside but can still leave deep marks. Emotional neglect, humiliation, chronic criticism, loss, fear, betrayal, lack of attuned care, medical trauma, workplace trauma, or ongoing threat can all affect a person’s sense of safety.
Trauma is not measured only by how dramatic an event appears. It is also measured by what the person’s system had to do to survive it.
We can start with what is happening in you now.
You do not have to tell the whole story all at once
Many people fear trauma therapy because they imagine they will have to describe everything in detail, revisit painful memories, or expose parts of themselves before they feel ready.
That is not how I work.
Trauma therapy does not have to begin with a full narrative of what happened. For some people, trying to tell the whole story too quickly can feel overwhelming, destabilising, or exposing.
We may begin instead with what is happening now: anxiety, shutdown, emotional flooding, numbness, dissociation, bodily tension, sleep disturbance, relationship difficulty, or the sense of never quite feeling safe.
The work may involve words, but it is not only a talking process. We may also pay attention to the body, nervous system, protective responses, relational patterns, parts of the self, and the meanings that became organised around the trauma.
The aim is not to force traumatic material into the open. It is to create enough safety for what has been held in survival mode to begin to shift.
How I work with trauma
My work with trauma is relational, body-aware, and tailored to the person in front of me.
I work openly and collaboratively, with transparency about the therapeutic direction and the pace of the work. We think together about what feels important, what feels manageable, and how therapy is unfolding.
I do not rush toward the deepest material. Often, the first task is helping the system become less overwhelmed, so that deeper work becomes possible without flooding, collapse, or shutdown.
I draw from an integrative background, but I do not apply techniques mechanically. The aim is to work in a way that fits your history, your wounds, your pace, and your capacity.
This may include:
relational work — how patterns formed and how they can show up between people
body-based trauma work — what your system does automatically under perceived threat
parts-informed work — working respectfully with protective strategies
nervous-system-informed work — supporting regulation, steadiness, and capacity
A core component of my trauma work is Deep Brain Reorienting (DBR), which works with underlying threat and orienting responses that may sit beneath more visible symptoms.
Depending on what is needed, I may also draw on Relational Transactional Analysis, Sensorimotor Psychotherapy, parts-informed work, EMDR-informed work, and, where helpful, ILF neurofeedback.
If you would like a fuller sense of the approaches I integrate in trauma work — and how they are used within one carefully paced process — you can read more here:
How trauma work usually unfolds
With support, time, and enough patience, the nervous system can become more balanced and flexible again.
In everyday life, that may mean less bracing, more rest, and more capacity to stay present under stress.
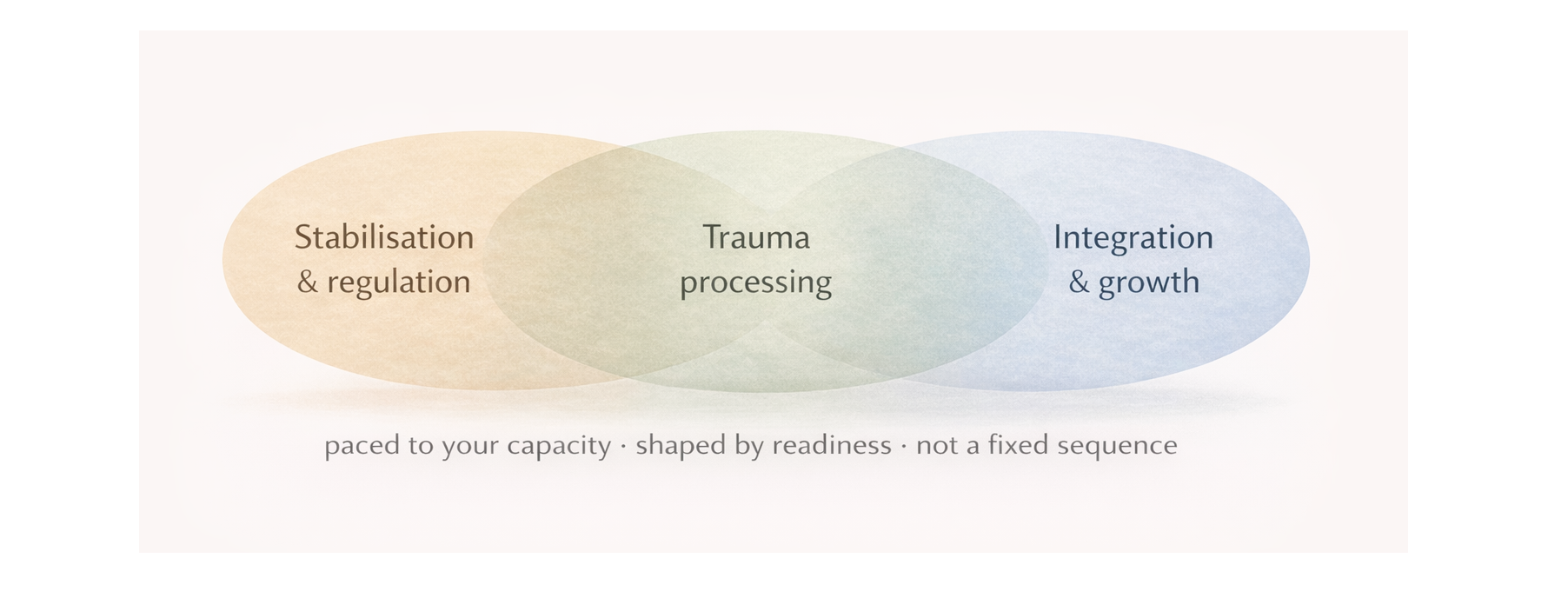
Trauma therapy often unfolds through three overlapping areas:
stabilisation and regulation
trauma processing
integration and growth
These are not rigid steps. Sometimes the work focuses mainly on stabilisation for a while. Sometimes deeper processing becomes possible sooner. Sometimes we move back and forth between processing, reflection, regulation, and integration.
This is not a failure of the work. It is often part of how careful trauma therapy needs to happen.
Where useful, I may also integrate ILF neurofeedback in person, either within our therapy or, in some cases, alongside work with another therapist or relevant clinician.
Read more about ILF neurofeedback ›
Trauma therapy with me is not a rapid processing model or a short intensive programme. I am not usually the right service for someone who is currently in acute crisis or who needs a level of support that weekly therapy alone cannot provide.
If you are unsure whether you are ready, that uncertainty is worth bringing. Readiness is something we can explore together.
For questions about pace, overwhelm, or how trauma-informed therapy begins, the FAQ may be helpful.
If you are considering trauma-focused therapy
If you are wondering whether this kind of work might help, you are very welcome to book a free 20-minute consultation.
You do not need to know exactly where to begin. We can talk about what has been happening in daily life, whether trauma feels central to what you are carrying, and whether this kind of work seems likely to help.
If you are unsure whether you are ready for trauma-focused work, that uncertainty is welcome. We can think about it together.
There is no pressure to continue beyond the consultation.
You may also find these pages helpful:
Individual psychotherapy ›
For a fuller sense of how I work in ongoing psychotherapy.
Symptoms & experiences ›
If you recognise trauma more through anxiety, shutdown, dissociation, relationship patterns, exhaustion, or overwhelm.
ILF neurofeedback ›
If sleep, overwhelm, reactivity, brain fog, or nervous-system instability are making daily life or therapy harder to manage.
Fees ›
For current fees and practical information.
Need urgent support now?
If you are in immediate danger, please call 999 or go to your nearest A&E.
If you need urgent emotional or crisis support, please visit:
Useful helplines and websites ›